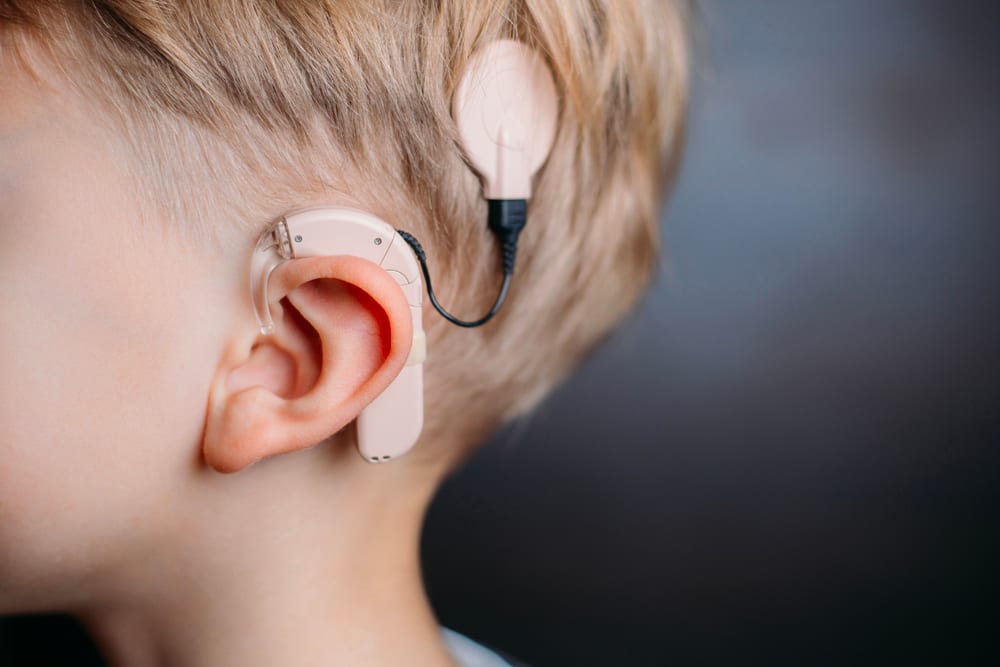
Cochlear Implantation

Duration
~2 hours

Downtime
2 weeks

Setting
Outpatient

Insurance
Covered

Lasts for
Long-lasting
Overview
Cochlear implant is an electronic device that stimulates the hearing nerve through electric pulses, bypassing the damaged inner ear. This allows patients to understand conversations and hear everyday-sounds again.
Why Consider Cochlear Implantation
There is a snail-shaped organ in our inner ear (cochlea) that stimulates the hearing nerve. Sometimes this organ gets damaged, genetically or because of infections, causing hearing loss.
The cochlear device bypasses this damage and stimulates the hearing nerve directly, which restores hearing.
The device works best for :
Individuals who have hearing loss on both sides or single-sided deafness with limited benefits from hearing aid.
Benefits
Improved hearing :
91% of patients reported hearing improvement. They were able to recognize words 46% better than before operation.
Improved social and mental wellbeing:
Cochlear implants enable meaningful social connections, open doors to employment and education, and significantly reduce the emotional burden and medical support many patients require.
Children’s educational improvement:
Children who received cochlear implants have better educational outcomes in reading, writing, and higher academic scores compared to children with similar hearing loss but with out cochlear implants.
Parts of the Cochlear Device
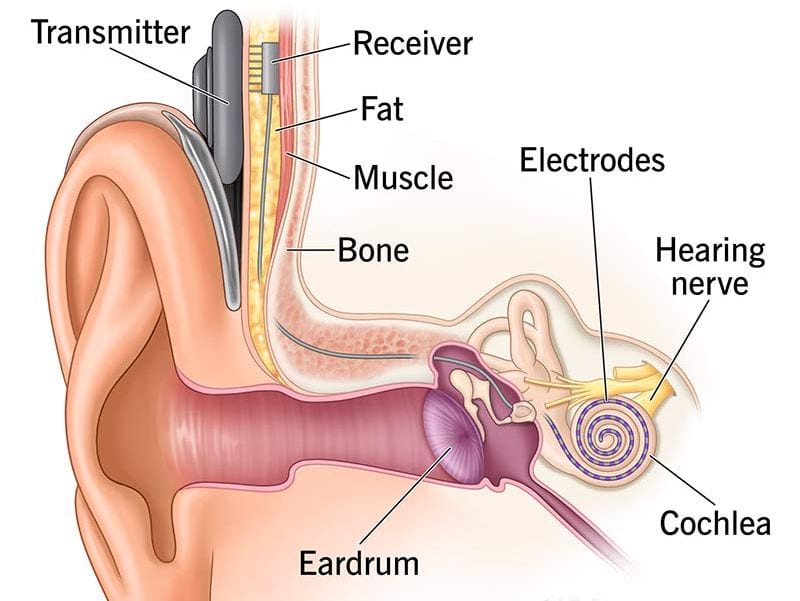
External part:
- Microphone: capture acoustic signals.
- Processor: transform acoustic to digital signals.
- Transmitter: sends digital signals to the receiver.
Internal part:
- Receiver: decode signals into electrical pulses.
- Electrodes: stimulate the hearing nerve.
Risks
2 to 9 people out of 100 experience major complications (like device failure and meningitis) after cochlear implantation while 2 to 10 people experience minor complications (like vertigo).
Complications | Rate |
|---|---|
Device failure | 4.7- 6.0 % |
Cerebrospinal fluid leak | 5% |
Vertigo | 2.5% |
Seroma | 1.8% |
Infection | 1.4% |
Electrode migration | 1.3% |
Meningitis | 0.07-0.19% |
Anesthesia
General Anesthesia
It is the most commonly used type and considered part of the standard care. You will be fully asleep during the procedure and won't feel anything.
Local Anesthesia
It is only used in adults and in cases when they can't tolerate general anesthesia.
Results & Rehabilitation
Hearing Improvement Timeline
Week 2-3
Detecting presence/absence of sound, distinguishing loud vs soft
Month 1
Beginning to differentiate speech from noise, recognizing familiar voices.
Month 2-3
Understanding simple conversations in quiet settings.
Month 3-6
Improved speech clarity, beginning phone use, and enjoying simple music.
Month 6-12
Continued refinement, better performance in background noise.
Auditory Training
Structured listening exercises begin immediately after activation. Daily practice with increasingly complex sounds progresses from environmental sounds to speech.
Speech and Language Therapy
This therapy is designed to help you interpret what you are hearing through the device into words and sentences. It also focuses on speech production, and for children, language development.
Adults typically require 3-6 months of weekly sessions. Children may need years of intensive therapy depending on age at implantation and previous language exposure.
Device Management Skills
Daily maintenance:
- Clean the external processor daily with a soft, dry cloth.
- Check and replace batteries as needed (typically on a weekly basis depending on battery type).
- Store the device in a protective case when not in use.
Signs of malfunction:
Watch for unusual sounds like buzzing, intermittent or complete loss of sound, physical damage to the processor, or battery draining faster than normal.
What to do:
If you notice any of these signs, first check that all connections are secure and try fresh batteries. If problems persist, contact your audiologist or cochlear implant center immediately. Keep spare parts on hand (extra batteries, cables, and a backup processor if possible) so you're never without your device while waiting for repairs.
Living with the Device
There will be some adjustments that patients need to tolerate with because of the device. These include:
- MRI restrictions will require alternative imaging or special protocols.
- Airport security procedures need advance planning.
- Water protection equipment for the device during swimming and bathing.
- Regular battery inventory and equipment backup planning.
Navigation: