Breast Reconstruction Surgery

Cost
$6,000–17,000

Duration
2-5 hours

Lasts for
Long Lasting

Downtime
6-8 Weeks

Setting
Inpatient/Outpatient
Overview
Breast reconstruction is a surgery that rebuilds the shape of the breast after its removal due to breast cancer or a high-risk genetic profile. It aims to re-create a breast mound that resembles the natural breast in form and size. It can also be used for patients born with an absent breast.
Who is Breast Reconstruction For?
After breast removal surgery, it is normal that cancer survivors feel self-conscious about changes in their body appearance.
Concern | Strength of Evidence |
|---|---|
After breast removal surgery | Well-Supported |
Asymmetrical breasts | Growing Evidence |
Absent breast since birth | Limited Evidence |
Inflammatory breast reconstruction | Disproven |
Benefits
Breast reconstruction offers the opportunity to restore the natural shape and symmetry of the breasts.
This means feeling whole, confident, and more comfortable in their clothing, in moments of intimacy, or simply when looking in the mirror. In cases where only one breast is removed, reconstruction can also address the discomfort and physical strain caused by the asymmetry and physical imbalance.
Procedure types
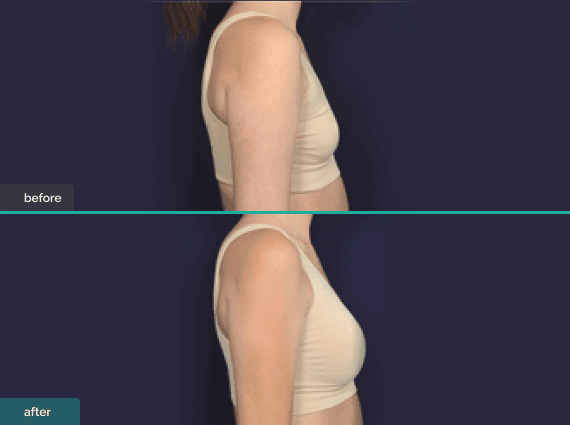
Implant-based Reconstruction
- 1-2 days
- Faster (4-8 weeks)
- Replacement every 10-15 years
Uses a breast implant (silicone or saline) to restore breast volume.
Pros
- Offers a variety of options in size, shape, and texture
- Shorter surgery time and faster recovery Katsuragi, R., Ozturk, C. N., Chida, K., Mann, G. K., Roy, A. M., Hakamada, K., Takabe, K., & Satake, T. (2024). Updates on Breast Reconstruction: Surgical Techniques, Challenges, and Future Directions. World Journal of Oncology, 15(6), 853–870. https://doi.org/10.14740/wjon1935
Cons
- Higher risk of complications;
- Some types offer a less natural look and feel Stefura, T., Rusinek, J., Wątor, J., Zagórski, A., Zając, M., Libondi, G., Wysocki, W. M., & Koziej, M. (2023). Implant vs. autologous tissue-based breast reconstruction: A systematic review and meta-analysis of the studies comparing surgical approaches in 55,455 patients. Journal of Plastic, Reconstructive & Aesthetic Surgery, 77, 346–358. https://doi.org/10.1016/j.bjps.2022.11.044
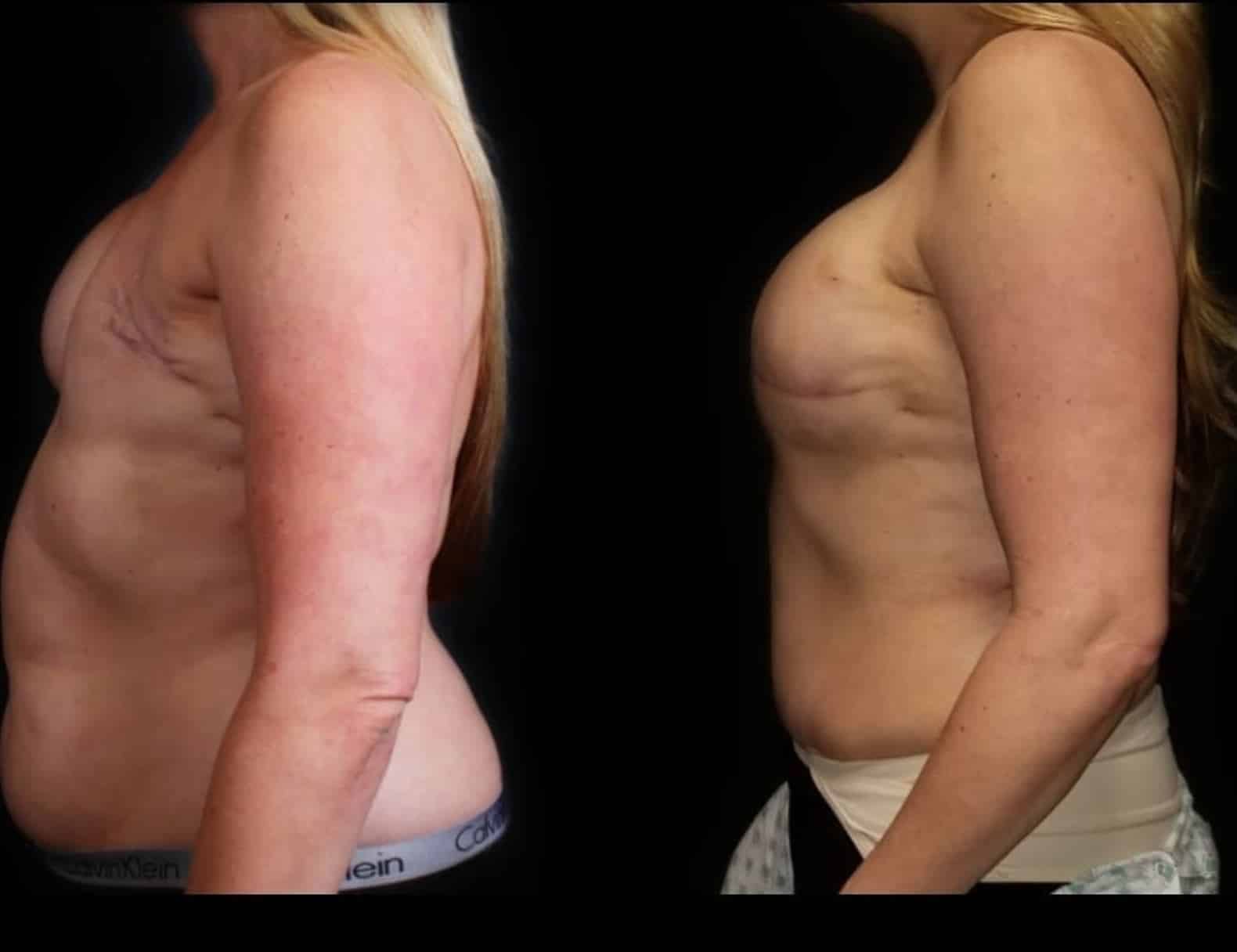
Flap-based Reconstruction
- 3-4 days
- Slower (6-12 weeks)
- Long-lasting
Uses tissue from another part of your body (donor site) — typically the abdomen, back, thigh, or buttock — to rebuild the breast. Sometimes microsurgery is done to reconnect blood vessels.
Pros
- Most natural look and feel
- Compatible with radiotherapy
- Potential body contouring at donor site
- Changes naturally with weight Katsuragi, R., Ozturk, C. N., Chida, K., Mann, G. K., Roy, A. M., Hakamada, K., Takabe, K., & Satake, T. (2024). Updates on Breast Reconstruction: Surgical Techniques, Challenges, and Future Directions. World Journal of Oncology, 15(6), 853–870. https://doi.org/10.14740/wjon1935
Cons
- Longer surgery and hospital stay
- Additional wound/scar at donor site
- Higher risk of bleeding
- Not suitable if prior surgery compromised donor site blood supply
- Higher cost Katsuragi, R., Ozturk, C. N., Chida, K., Mann, G. K., Roy, A. M., Hakamada, K., Takabe, K., & Satake, T. (2024). Updates on Breast Reconstruction: Surgical Techniques, Challenges, and Future Directions. World Journal of Oncology, 15(6), 853–870. https://doi.org/10.14740/wjon1935 Stefura, T., Rusinek, J., Wątor, J., Zagórski, A., Zając, M., Libondi, G., Wysocki, W. M., & Koziej, M. (2023). Implant vs. autologous tissue-based breast reconstruction: A systematic review and meta-analysis of the studies comparing surgical approaches in 55,455 patients. Journal of Plastic, Reconstructive & Aesthetic Surgery, 77, 346–358. https://doi.org/10.1016/j.bjps.2022.11.044
Hybrid Reconstruction
- 2-6 days
- 4-8 weeks
- 10-15 years ( implant component)
Combines an implant with your own tissue. Used when the desired breast size exceeds what tissue alone can provide, or when donor sites are limited.
Best for:
- Thin patients with insufficient donor tissue
- Bilateral reconstruction
- When natural tissue coverage is needed over an implant
Considerations:
- Combines benefits of both approaches but also carries risks of both
- Implant component will need replacement
- Requires specialized surgical expertise
Combined Procedures
Breast reconstruction can be combined with lymphatic reconstruction surgery to avoid arm swelling, or nerve reconstruction to restore breast sensation.
When the flap is taken from the abdomen, it can be combined with abdominoplasty for body contouring.
Reconstruction Timeline
Breast reconstruction involves multiple stages over 6–12 months, depending on the type of procedures and whether you need other cancer treatments in between.
- Initial Reconstruction Surgery
Implant, flap, or device to expand skin and prepare for future implants. - Chemotherapy / Radiotherapy
If needed, cancer treatment takes place between reconstruction stages. - Revisional Surgery (3 months after)
Refining shape, injecting fat for smoother texture, balancing procedure on the other breast (reduction, lifting, or augmentation). - Nipple and Areola Reconstruction (3-4 months later, variable)
Nipple and areola reconstruction or tattooing to complete the final appearance.
Timing of the first reconstruction
Immediate Reconstruction
Happens at the same day of breast removal
Pros:
- Minimizes the psychological impact of not having breasts, even if temporarily Roy, N., Downes, M. H., Ibelli, T., Amakiri, U. O., Li, T., Tebha, S. S., Balija, T. M., Schnur, J. B., Montgomery, G. H., & Henderson, P. W. (2024). The psychological impacts of post-mastectomy breast reconstruction: A systematic review. Annals of Breast Surgery, 8, 19–19. https://doi.org/10.21037/abs-23-33
- Better cosmetic results (the surgeon can preserve breast skin and nipple) Faster recovery,
- Fewer number of surgeries and lower cost.
Cons:
- Having post-operative chemotherapy, radiotherapy, or cancer recurrence can affect the reconstruction results Thamm, O. C., & Andree, C. (2018). Immediate Versus Delayed Breast Reconstruction. Clinics in Plastic Surgery, 45(1), 119–127. https://doi.org/10.1016/j.cps.2017.08.010
Delayed Reconstruction
Happens months to years after breast removal
Pros:
- Avoids interference between reconstruction results and post-operative chemotherapy/radiotherapy (surgery is delayed after treatment is completed);
- Since most cancer recurrence occurs in the first 1-2 years, delaying reconstruction ensures the patient is free of cancer to optimize the reconstruction results;
- You have more time to weigh your options and make your decision.
Cons:
- Psychological impact, due to the temporary lack of breasts;
- Scar tissue from breast removal surgery makes reconstruction more challenging and limits your options;
- Cosmetic results may not be as optimal as immediate reconstruction (less skin is remaining) Thamm, O. C., & Andree, C. (2018). Immediate Versus Delayed Breast Reconstruction. Clinics in Plastic Surgery, 45(1), 119–127. https://doi.org/10.1016/j.cps.2017.08.010 Yoon, A. P., Qi, J., Brown, D. L., Kim, H. M., Hamill, J. B., Erdmann-Sager, J., Pusic, A. L., & Wilkins, E. G. (2018). Outcomes of immediate versus delayed breast reconstruction: Results of a multicenter prospective study. Breast (Edinburgh, Scotland), 37, 72–79. https://doi.org/10.1016/j.breast.2017.10.009
Results
Aesthetic results can vary even when surgery is performed without complications.
Favorable Result
- Near-natural breast shape and contour
- Natural feel and physical comfort with no tightness or pulling sensation
- Symmetrical breasts that match in size, shape, and position on the chest
- Full or near-full shoulder range of movement

Unfavorable Result
- Breast shape appears unnatural or asymmetrical
- Tightness or pulling sensation persists
- Limited shoulder range of movement

Risks
Who Can’t Undergo Breast Reconstruction?
Breast removal after inflammatory breast cancer because of its aggressive nature and the need for extensive radiotherapy and chemotherapy before and after surgery.
Risk Factors
- Radiotherapy
Higher risk of complications, especially with implant-based reconstruction - Post-operative chemotherapy/radiotherapy
Can affect reconstruction results Thamm, O. C., & Andree, C. (2018). Immediate Versus Delayed Breast Reconstruction. Clinics in Plastic Surgery, 45(1), 119–127. https://doi.org/10.1016/j.cps.2017.08.010 - Cancer recurrence
Sometimes, cancer may recur especially in the first two years after breast cancer treatment. This can compromise reconstruction results because of the treatment needed to address the new cancer.
Chapter references
- 1
- 2
- 3
- 4
- 5
Navigation: